Researching MRSA
Staphylococcus aureus is capable of causing numerous types of infections in humans that range from mild to serious. Indeed, S. aureus can cause minor skin infections such as boils or it can cause more serious infections that result in clinical manifestations such as endocarditis, osteomyelitis, arthritis, septicemia, and toxic shock syndrome, among others, as well as infections of surgical wounds. What is more, S. aureus is known as one of the so-called superbugs, because of the pathogenic nature of the bacterium combined with the fact that it frequently acquires resistance to many currently used antibiotics. Methicillin resistant S. aureus, or MRSA, is one of the most notorious pathogens in the hospital environment and the spread of community acquired MRSA is now becoming prevalent.
The Heinrichs lab investigates the molecular basis of MRSA infections, with a special focus on the mechanisms MRSA uses to acquire growth promoting nutrients, and how these processes govern pathogenicity. Using a wide range of molecular and biochemical tools, the lab aims to answer the following questions:
how does MRSA regulate nutrient source preference?
how does mrsa liberate nutrients from the host?
How does inhibiting nutrient acquisition pathways affect the outcome of MRSA infection?
What are mechanisms by which competing microbes naturally interfere with MRSA?
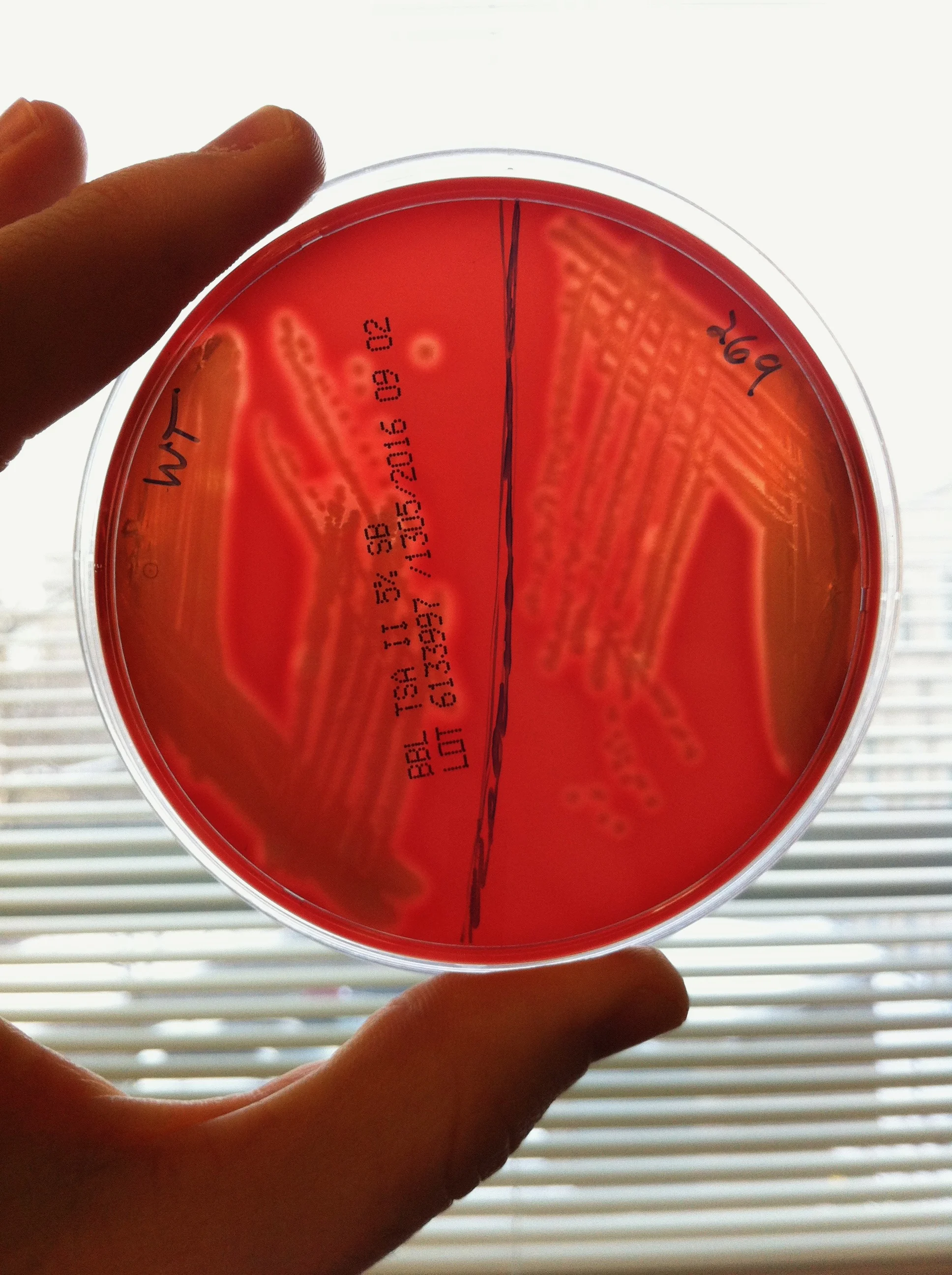
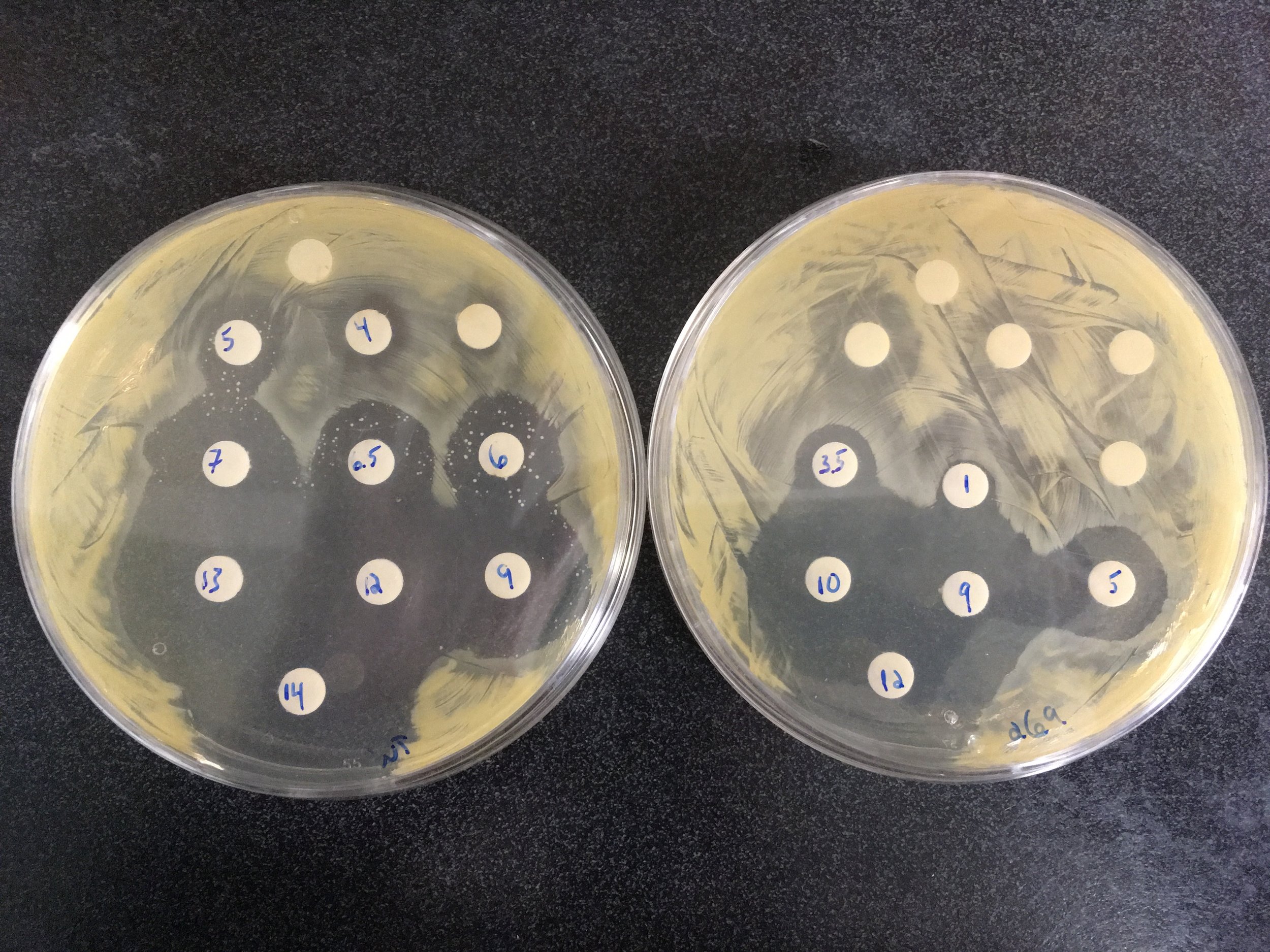
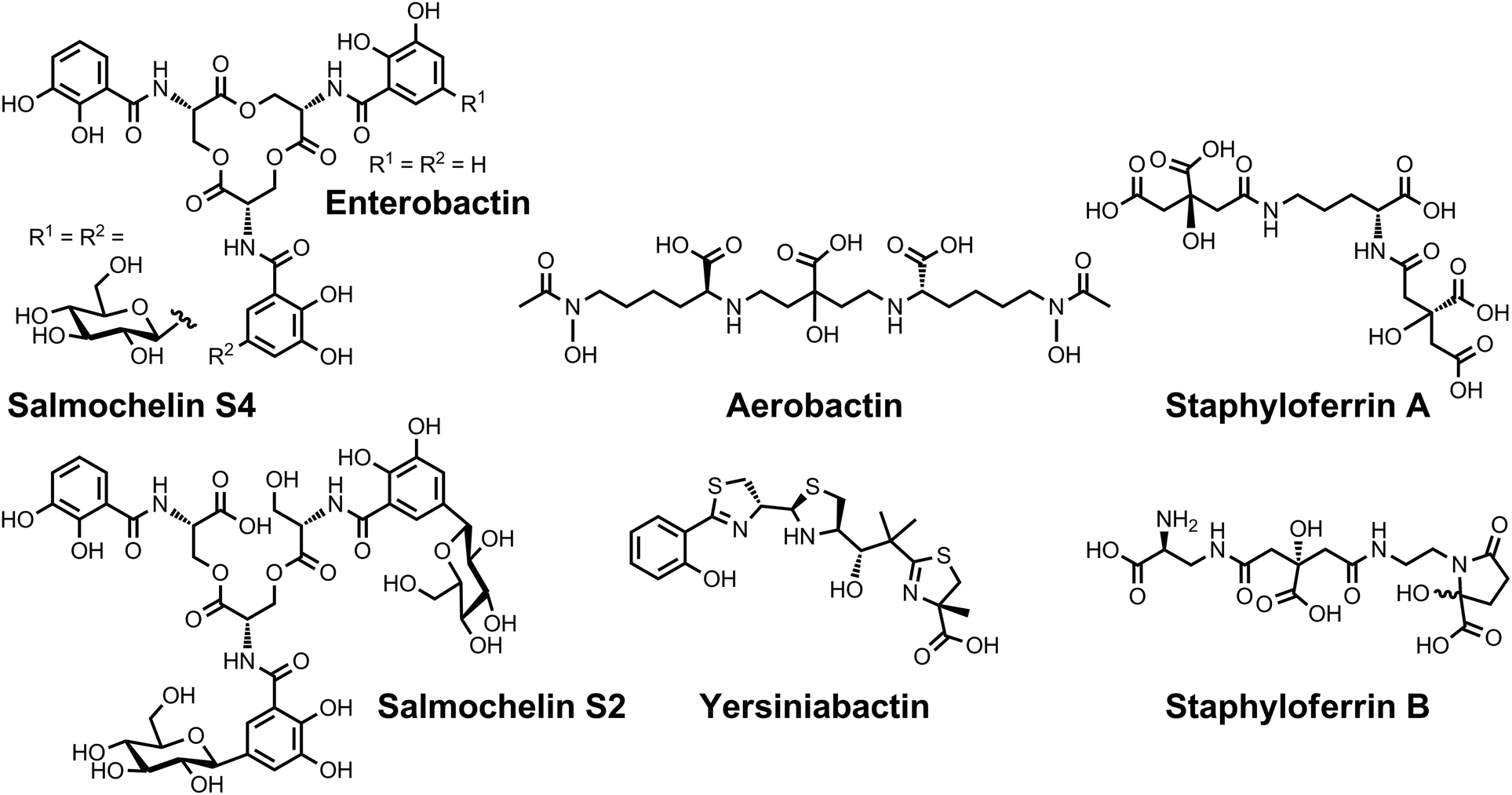

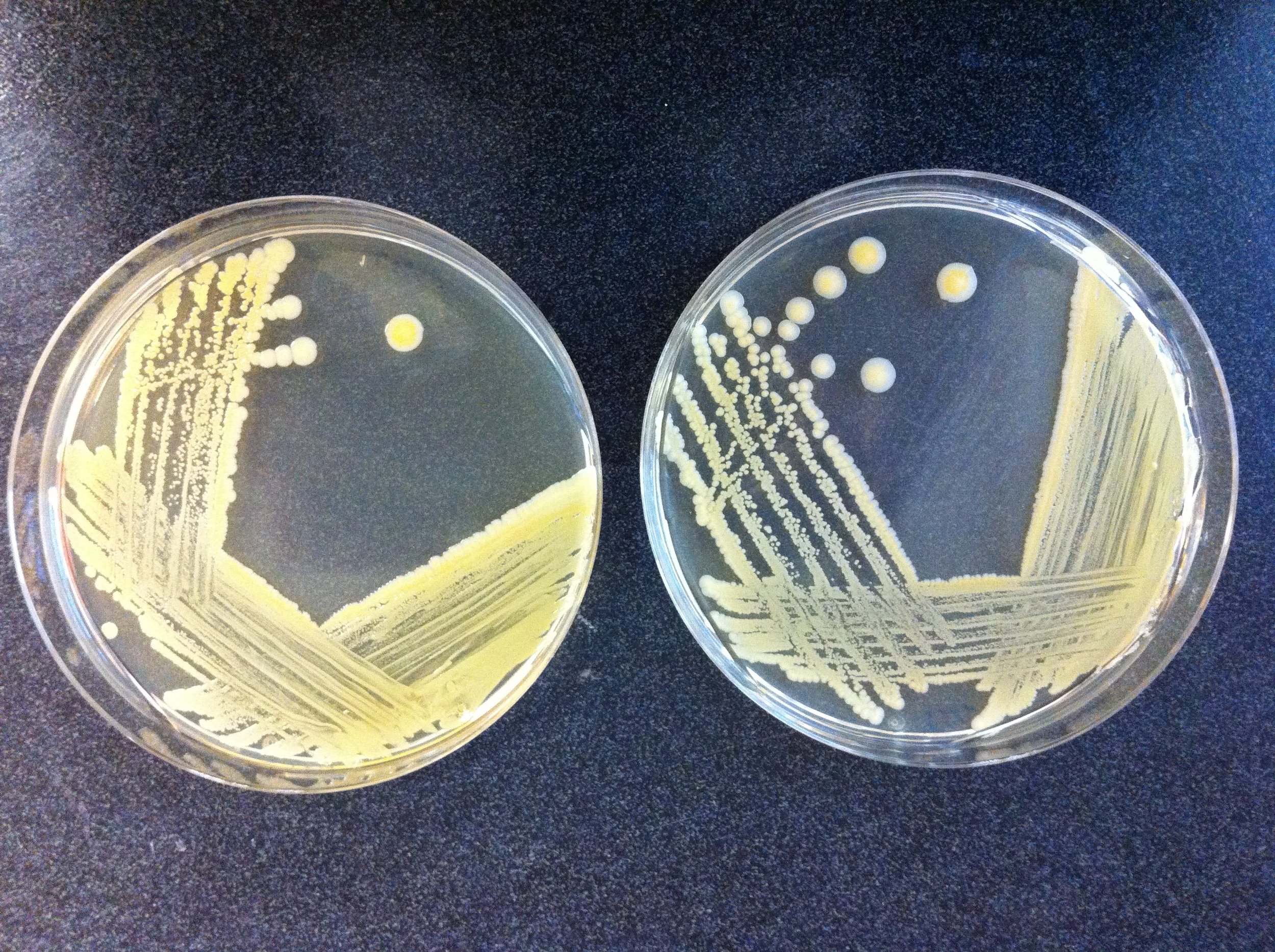
SelectED RECENT Publications
Moldovan A, Flannagan RS, Rühling M, Stelzner K, Hans C, Paprotka K, Kunz TC, Heinrichs DE, Rudel T, Fraunholz MJ. Inactivation of branched-chain amino acid uptake halts Staphylococcus aureus growth and induces bacterial quiescence within macrophages. 2025. PLoS Pathog. 2025 Aug 8;21(8):e1013291. doi: 10.1371/journal.ppat.1013291. eCollection 2025 Aug. PMID: 40779604.
Gaudreau A, Watson DW, Flannagan RS, Roy P, Shen C, Abdelmoneim A, Beavers WN, Gillies ER, El-Halfawy OM, Heinrichs DE. Mechanistic insights and in vivo efficacy of thiosemicarbazones against methicillin-resistant Staphylococcus aureus. Journal of Biological Chemistry. 2024 Oct;300(10):107689. doi: 10.1016/j.jbc.2024.107689. Epub 2024 Aug 17. PMID: 39159815.
Xiong YQ, Li Y, Goncheva MI, Elsayed AM, Zhu F, Li L, Abdelhady W, Flannagan RS, Yeaman MR, Bayer AS, Heinrichs DE. The Purine Biosynthesis Repressor, PurR, Contributes to Vancomycin Susceptibility of Methicillin-resistant Staphylococcus aureus in Experimental Endocarditis. Journal of Infectious Diseases. 2024 Jun 14;229(6):1648-1657. doi: 10.1093/infdis/jiad577. PMID: 38297970.
Fauerharmel-Nunes T, Flannagan RS, Goncheva MI, Bayer AS, Fowler VG Jr, Chan LC, Yeaman MR, Xiong YQ, Heinrichs DE. MRSA Isolates from Patients with Persistent Bacteremia Generate Nonstable Small Colony Variants In Vitro within Macrophages and Endothelial Cells during Prolonged Vancomycin Exposure. Infect Immun. 2023 Jan 24;91(1):e0042322. doi: 10.1128/iai.00423-22. Epub 2023 Jan 5. PubMed PMID: 36602380; PubMed Central PMCID: PMC9872686.
Goncheva MI, Gibson RM, Shouldice AC, Dikeakos JD, Heinrichs DE. The Staphylococcus aureus protein IsdA increases SARS CoV-2 replication by modulating JAK-STAT signaling. iScience. 2023 Feb 17;26(2):105975. doi: 10.1016/j.isci.2023.105975. Epub 2023 Jan 13. PubMed PMID: 36687318; PubMed Central PMCID: PMC9838083.
Chin D, Flannagan RS, Tuffs SW, Chan JK, McCormick JK, Heinrichs DE. Staphylococcus lugdunensis Uses the Agr Regulatory System to Resist Killing by Host Innate Immune Effectors. Infect Immun. 2022 Oct 20;90(10):e0009922. doi: 10.1128/iai.00099-22. Epub 2022 Sep 7. PubMed PMID: 36069592; PubMed Central PMCID: PMC9584346.
Goncheva MI, Chin D, Heinrichs DE. Nucleotide biosynthesis: the base of bacterial pathogenesis. Trends Microbiol. 2022 Aug;30(8):793-804. doi: 10.1016/j.tim.2021.12.007. Epub 2022 Jan 22. Review. PubMed PMID: 35074276.
Flannagan RS, Brozyna JR, Kumar B, Adolf LA, Power JJ, Heilbronner S, Heinrichs DE. In vivo growth of Staphylococcus lugdunensis is facilitated by the concerted function of heme and non-heme iron acquisition mechanisms. J Biol Chem. 2022 May;298(5):101823. doi: 10.1016/j.jbc.2022.101823. Epub 2022 Mar 10. PubMed PMID: 35283192; PubMed Central PMCID: PMC9052147.
Tuffs SW, Goncheva MI, Xu SX, Craig HC, Kasper KJ, Choi J, Flannagan RS, Kerfoot SM, Heinrichs DE, McCormick JK. Superantigens promote Staphylococcus aureus bloodstream infection by eliciting pathogenic interferon-gamma production. Proc Natl Acad Sci U S A. 2022 Feb 22;119(8). doi: 10.1073/pnas.2115987119. PubMed PMID: 35165181; PubMed Central PMCID: PMC8872782.



